In Da Nang, health facilities have recently recorded five severe poisoning cases linked to the consumption of fermented fish, a staple in many family meals.
According to Dr Nguyen Trung Nguyen, Director of the Poison Control Center at Bach Mai Hospital in Hanoi, botulinum toxin is one of the most potent neurotoxins known, produced by the bacterium Clostridium botulinum. This bacterium thrives in anaerobic environments - those lacking oxygen - commonly found in sealed, fermented or improperly stored foods. Once inside the body, the toxin can cause muscle paralysis, respiratory failure and can be fatal without timely treatment.
Vietnam has documented several serious botulinum poisoning incidents related to homemade foods. In 2020, a family in Quang Nam was hospitalized after consuming home-fermented carp, exhibiting symptoms such as drooping eyelids, difficulty speaking and limb weakness, with some requiring prolonged mechanical ventilation.
In 2023, a cluster of severe cases occurred in Ho Chi Minh City after people consumed fermented fish and homemade paste, with many patients treated at Cho Ray Hospital suffering progressive paralysis and respiratory failure. In 2024, a similar case was reported in Binh Duong after a family consumed fermented snakehead fish.
Associate Professor Nguyen Duy Thinh, former lecturer at the Institute of Food Technology, Hanoi University of Science and Technology, noted that protein-rich foods such as meat and fish are particularly vulnerable to bacterial contamination, especially when fermented or sealed under unhygienic conditions. Manual processing without proper control of temperature and environment can create ideal conditions for anaerobic bacteria to grow.
Most concerning is that food contaminated with botulinum toxin often shows no signs of spoilage - no unusual odor, discoloration or slimy texture - making it extremely difficult for consumers to detect and increasing the risk of accidental poisoning.
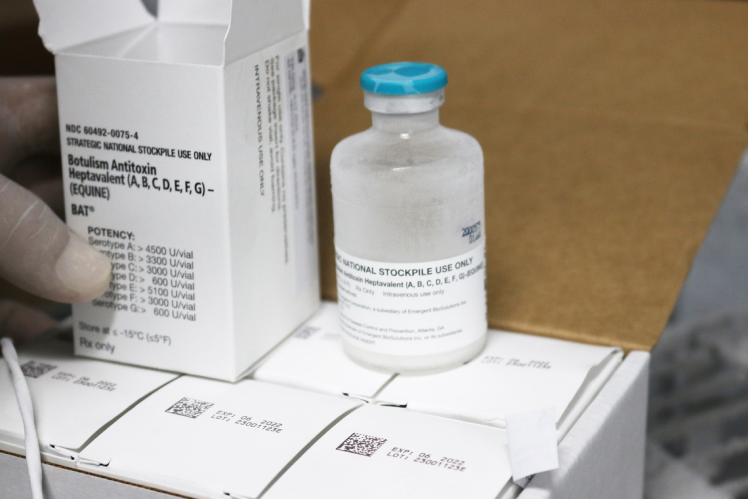
A major challenge in treating botulinum poisoning is the scarcity and high cost of the specific antidote, Botulinum Antitoxin (BAT). According to health authorities, the drug is not readily available in many facilities in Vietnam and often must be urgently supplied by the World Health Organization from international stockpiles in Geneva. Each vial costs about US$8,000 (approximately VND200 million) and must be transported quickly to be effective.
Dr Nguyen Trung Nguyen emphasized that there is currently no alternative to BAT. If administered within the “golden window” of 48 to 72 hours after symptom onset, patients who require mechanical ventilation for one to two days may recover more quickly, potentially coming off ventilators within five to seven days and beginning rehabilitation early. However, delayed detection can result in prolonged, complex treatment with significant risks.
Due to the relatively low number of cases and the high cost, hospitals face difficulties in maintaining stockpiles of the antidote, making prevention especially critical.
High-risk foods include homemade canned products, fermented fish and meat, fish sauce, pickled vegetables, pate, sausages and other sealed foods stored for long periods. To reduce risk, experts advise following strict food safety practices, avoiding products that are swollen, dented, rusted or have unusual odors. It is also recommended to boil or steam canned foods for at least 10 minutes before consumption to neutralize toxins.
In particular, if symptoms such as drooping eyelids, muscle weakness, difficulty swallowing or speaking occur after consuming suspected foods, individuals should seek immediate medical attention for timely diagnosis and treatment.
Phuong Thuy